Ask ten people what “normal” looks like, and you’ll get a dozen answers. When someone’s mood, behaviour, or functioning shifts, it’s tempting to use language that labels the person or their behaviour as not normal.
But from a treatment and recovery perspective, normal is a tricky thing to pin down, and probably a far less useful label than we think. In today’s article, we discuss the problem with “normal” and what we can focus on instead.
Normal Isn’t a Fixed Point — It’s a Continuum
Mental health works a lot like physical health: we’re not either healthy or ill in one neat box. Instead, most experts describe mental health as a continuum that moves with life stressors, available supports, our own biology, and time.
A well-known continuum-based model is the Mental Health Continuum Model, which emerged sometime around 2007, during a period when Canada’s military and public health sectors were rethinking how to address operational stress injuries, PTSD, and stigma among service members and first responders.
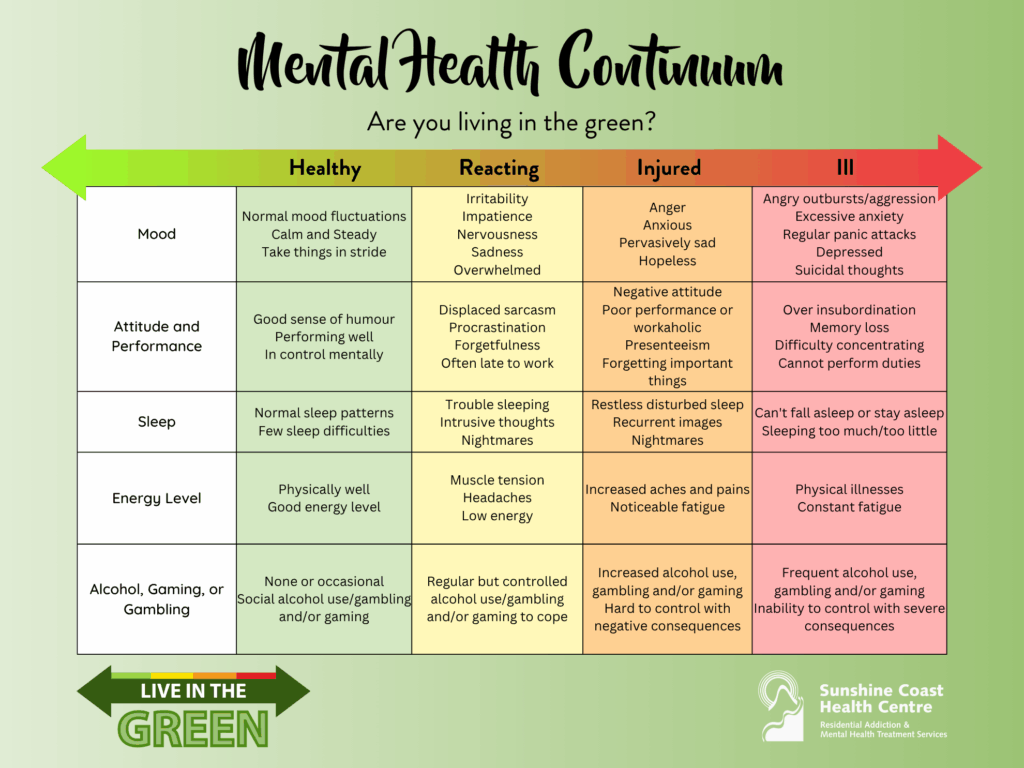
Another continuum-based model is the dual continua model, which views mental illness and mental well-being as two separate but related dimensions; In other words, it shows that someone can experience symptoms of mental illness while still maintaining aspects of positive well-being, or have no diagnosable illness yet still struggle with low well-being.
Used widely across many Canadian programs, this model helps clinicians spot early changes before problems become diagnosable illnesses, and shows why someone can be struggling one week and coping better the next. Crucially, the model reframes normal from a rigid standard into a range of human experiences.
The Numbers Show Variability, Not Exception
If you worry that struggling means you’re abnormal, the data is a kinder mirror. About one in five Canadians experiences a mental illness in any given year, and by the time we reach middle age, half of us will have had a diagnosable condition at some point.
Large, recent national studies also show millions of people living with mood, anxiety or substance-use disorders, and many more with subclinical stress and distress. Those numbers tell us that variability in mood and behaviour is common, not rare. Knowing this makes reaching for help feel less like an admission of failure and more like a normal part of being human.
“Normal” Can Be a Barrier to Help
When families say “we just want them to be normal again,” it can come from love… but it can also set unrealistic expectations. Expecting a rapid return to a former baseline can create shame when recovery takes time or when a new baseline emerges.
Research shows that stigma around mental health fuels silence, delays treatment, and increases isolation; that’s why public education, such as calling out myths and offering factual frames, matters so much. Shifting the conversation from “fixing normal” to “supporting health” opens the door to early help and sustainable recovery.
Recovery Looks Different For Different People
Healing stories in our treatment centre remind us that recovery is often nonlinear. One client we worked with described it like learning to swim after being tossed in cold water: the first goal was to stop drowning, then to float, and later to swim confidently again.

For some people, recovery restores previous functioning. For other folks, it creates a new, healthier normal that includes ongoing supports and coping strategies. Both outcomes are valid and real.
Practical Steps For Families Who Want to Help
The language we use is important. Start by replacing the word normal with concrete goals:
- Better sleep
- Fewer panic attacks
- Safer substance use
- Improved communication
Educating ourselves with trusted sources and tools that explain the mental health continuum and common symptoms can improve our understanding. Encourage early help, as brief interventions and therapy are most effective when started sooner rather than later. And practice compassion for the person struggling and for yourself.
It’s important to remember that normal is more of an abstract social concept than a clinical target. Because mental health lives on a continuum, the better question than “Is this normal?” is “Is this manageable, and what supports help?”
When families move from judgment to curiosity and from labels to concrete goals, they find pathways to recovery that are realistic, humane, and sustainable. You don’t have to fit a past version of normal to be well… you just need help that fits you.
When to Seek Professional Support
If distress is persistent, interferes with daily functioning, or includes thoughts of self-harm, it’s crucial to seek professional support. A clinician can map where someone sits on the continuum, suggest evidence-based interventions, and involve family where appropriate. Treatment can be brief or long-term, medical, or psychosocial. What matters is matching care to need, not fitting a person back into some imagined or constructed normal.

Sunshine Coast Health Centre and Georgia Strait Women’s Clinic are world-class centres for addiction treatment and mental health. We take an approach that recognizes the importance of the physical, psychological, social and spiritual aspects of individuals in treatment and recovery. If you or someone you know is struggling with substance use or mental health, give us a call today.



